保留活動之脊椎手術
文/台北榮總神經外科 吳昭慶醫師
進步的現代脊椎手術觀念包含三大原則:
- 放鬆受壓迫的神經
- 穩定病變的脊椎節段
- 平衡整體脊椎的排列與支撐12。
最常見的脊椎手術治療腰椎間盤突出,僅須切除椎間軟骨突出的部分,就可藉此改善神經被壓迫造成的腿部痠痛無力,然而有些時候除了減壓神經外,還需要加上植入物(例如支架或螺釘等),來增強脊椎穩定度,譬如發生腰椎滑脫症時,方能解決神經壓迫和脊椎骨脫位造成的腰痠背痛及行動困難。
另外還有少部分病人,因罹患嚴重的脊椎側彎,造成胸廓體態變形,往往需要手術來矯正其異常扭轉排列的脊椎骨,這種嚴重的狀況則幾乎都必須作多節段的脊椎內固定骨融合手術,才能維持手術成效,雖然大多數這類病人術後皆達到顯著的進步,但這類多節段(五節以上、甚至拾節以上)的骨融合內固定手術畢竟跟原本生理構造差距不小(造成多節脊椎骨融合而不再能彎曲),勢必造成日後脊椎其他的問題,例如鄰近節病變等。
因此,現代科技發展出保留活動之脊椎手術,在部分脊椎疾病的治療時,可以避免傳統的骨融合及內固定。
雖然這類保留活動的脊椎手術至今無法完全取代所有的內固定骨融合手術,但卻可以解決某些脊椎疾病,提供特定病人族群一種更接近生理狀態(活動)的治療選擇。
近幾年來頸椎人工椎間盤置換術之使用與日俱增,目前也已經有許多美國FDA的臨床試驗證據支持,對於壹節或貳節的頸椎退化性椎間盤疾病,當保守療法(藥物或物理治療)無效時,可以考慮使用頸椎人工椎間盤置換術之手術治療,相較於傳統的前位頸椎間盤切除及內固定骨融合術而言。
除了可以同樣解決神經壓迫外,人工椎間盤手術更能保留頸椎的活動度(3,11,13,15,16),在長達五至七年的臨床追蹤後1,8-10,18,發現這樣的頸椎人工椎間盤置換術能得到與傳統骨融合術相同或更佳的症狀改善、神經學進步,雖然其對於鄰近節病變的保護效果仍然不確定,但顯然頸椎人工椎間盤應該是相當安全有效、又能保留活動之脊椎手術策略。
雖然人工椎間盤在頸椎似乎很有價值,不過這樣的良好療效並不能推廣到腰椎,相對更常見的腰椎間盤凸出所造成坐之骨神經痛,目前的臨床試驗證據並不足以支持腰椎人工椎間盤的廣泛應用17,主要因為縱使腰椎人工椎間盤的臨床試驗起始更早,但至今仍缺乏長期有效的證據,且它的手術取出路徑較為困難危險,故當代人工椎間盤手術在腰椎之應用仍非常侷限。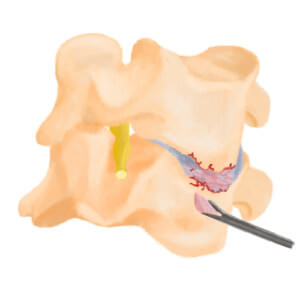
退化的頸椎與椎間盤
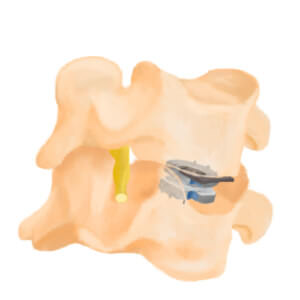
頸椎人工椎間盤
常見的腰椎手術若牽涉脊椎支撐的穩定度疑慮,則可以考慮使用一些材料和植入物來輔助增強其穩定度,除骨融合(包含傳統與微創)內固定外,尚有一些特意設計來保留活動度的器材,這些保留活動度的手術策略主要分為兩大類植入器材: 以椎弓根螺釘為基礎的彈性穩定器、或各式棘突間的支撐器。
其中腰椎動態穩定系統即為前者之代表,國內外學者(含筆者)曾發表數篇論文2,4-7,14,顯示其臨床效果跟傳統骨融合固定手術相近,可以保留一定比例之腰椎活動度,過去曾有其他學者質疑之螺釘鬆脫問題似乎也不影響結果,故對於欲增強穩定度之腰椎手術,此腰椎動態穩定系統應該是個值得考慮的選擇。
然而,對於各式棘突間的支撐器(interspinous devices)之適應症,則目前缺乏普遍的共識,雖有一些臨床試驗證明其安全有效,但真正最適合的使用時機還不十分明確,通常認為它有利於製造局部腰椎的前彎,而各式設計又提供不同程度的穩定。
是故上述這些器材都還須更多的臨床經驗來證明其療效。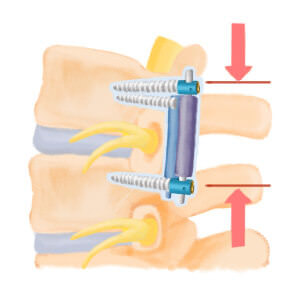
腰椎動態穩定系統
保留活動之脊椎手術 (Spinal Motion Preservation Surgery)必然是當今脊椎手術的發展方向,前文中所提及的這些器材,包含人工椎間盤、椎弓根螺釘為基礎的彈性穩定器、或各式棘突間的支撐器,其實都已經得到一些相當不錯的臨床使用經驗,在慎選的某些病症、特定部分的脊椎疾病、並且配合精準的手術。
許多病人也能因此得到症狀改善、神經學進步。唯這類器材普遍存在一基本問題,即是對於其耐用性及磨耗之疑慮12,但就如同其他傳統的骨融合手術一般,沒有任何一樣治療方式是完美無瑕的,畢竟這些手術修理的技術都無法使人返老還童,也無法重造出天然的人體結構,故還是必須提倡生理保健,並持續專注臨床研究,期待未來能有更多臨床證據、更新的治療技術、以達更高的病人滿意度。
吳昭慶 改寫自http://www.hindawi.com/journals/bmri/2015/372502/
參考文獻
- Burkus JK, Traynelis VC, Haid RW, Jr., Mummaneni PV: Clinical and radiographic analysis of an artificial cervical disc: 7-year follow-up from the Prestige prospective randomized controlled clinical trial: Clinical article. J Neurosurg Spine 21:516-528, 2014
- Fay LY, Chang PY, Wu JC, Huang WC, Wang CH, Tsai TY, et al: Dynesys dynamic stabilization-related facet arthrodesis. Neurosurg Focus 40:E4, 2016
- Fay LY, Huang WC, Wu JC, Chang HK, Tsai TY, Ko CC, et al: Arthroplasty for cervical spondylotic myelopathy: similar results to patients with only radiculopathy at 3 years’ follow-up. J Neurosurg Spine 21:400-410, 2014
- Fay LY, Wu JC, Tsai TY, Tu TH, Wu CL, Huang WC, et al: Intervertebral disc rehydration after lumbar dynamic stabilization: magnetic resonance image evaluation with a mean followup of four years. Adv Orthop 2013:437570, 2013
- Fay LY, Wu JC, Tsai TY, Wu CL, Huang WC, Cheng H: Dynamic stabilization for degenerative spondylolisthesis: evaluation of radiographic and clinical outcomes. Clin Neurol Neurosurg 115:535-541, 2013
- Ko CC, Tsai HW, Huang WC, Wu JC, Chen YC, Shih YH, et al: Screw loosening in the Dynesys stabilization system: radiographic evidence and effect on outcomes. Neurosurg Focus 28:E10, 2010
- Kuo CH, Chang PY, Wu JC, Chang HK, Fay LY, Tu TH, et al: Dynamic stabilization for L4-5 spondylolisthesis: comparison with minimally invasive transforaminal lumbar interbody fusion with more than 2 years of follow-up. Neurosurg Focus 40:E3, 2016
- Loumeau TP, Darden BV, Kesman TJ, Odum SM, Van Doren BA, Laxer EB, et al: A RCT comparing 7-year clinical outcomes of one level symptomatic cervical disc disease (SCDD) following ProDisc-C total disc arthroplasty (TDA) versus anterior cervical discectomy and fusion (ACDF). Eur Spine J, 2016
- Mummaneni PV, Amin BY, Wu JC, Brodt ED, Dettori JR, Sasso RC: Cervical artificial disc replacement versus fusion in the cervical spine: a systematic review comparing long-term follow-up results from two FDA trials. Evid Based Spine Care J 3:59-66, 2012
- Murrey D, Janssen M, Delamarter R, Goldstein J, Zigler J, Tay B, et al: Results of the prospective, randomized, controlled multicenter Food and Drug Administration investigational device exemption study of the ProDisc-C total disc replacement versus anterior discectomy and fusion for the treatment of 1-level symptomatic cervical disc disease. Spine J 9:275-286, 2009
- Upadhyaya CD, Wu JC, Trost G, Haid RW, Traynelis VC, Tay B, et al: Analysis of the three United States Food and Drug Administration investigational device exemption cervical arthroplasty trials. J Neurosurg Spine 16:216-228, 2012
- Wu JC, Hsieh PC, Mummaneni PV, Wang MY: Spinal Motion Preservation Surgery. Biomed Res Int 2015:372502, 2015
- Wu JC, Huang WC, Tsai HW, Ko CC, Fay LY, Tu TH, et al: Differences between 1- and 2-level cervical arthroplasty: more heterotopic ossification in 2-level disc replacement: Clinical article. J Neurosurg Spine 16:594-600, 2012
- Wu JC, Huang WC, Tsai HW, Ko CC, Wu CL, Tu TH, et al: Pedicle screw loosening in dynamic stabilization: incidence, risk, and outcome in 126 patients. Neurosurg Focus 31:E9, 2011
- Wu JC, Huang WC, Tsai TY, Fay LY, Ko CC, Tu TH, et al: Multilevel arthroplasty for cervical spondylosis: more heterotopic ossification at 3 years of follow-up. Spine (Phila Pa 1976) 37:E1251-1259, 2012
- Wu JC, Huang WC, Tu TH, Tsai HW, Ko CC, Wu CL, et al: Differences between soft-disc herniation and spondylosis in cervical arthroplasty: CT-documented heterotopic ossification with minimum 2 years of follow-up. J Neurosurg Spine 16:163-171, 2012
- Wu JC, Tu TH, Mummaneni PV: Spinal arthroplasty: differences between the cervical and lumbar spine. World Neurosurg 78:245-246, 2012
- Zigler JE, Delamarter R, Murrey D, Spivak J, Janssen M: ProDisc-C and anterior cervical discectomy and fusion as surgical treatment for single-level cervical symptomatic degenerative disc disease: five-year results of a Food and Drug Administration study. Spine (Phila Pa 1976) 38:203-209, 2013




